Study: African American men less likely to use targeted prostate cancer detection method
UC research shows that African American men receive MRI-ultrasound biopsies less than white men
Researchers at the University of Cincinnati have found in a retrospective study that African American men are less likely to use a more targeted biopsy option for prostate cancer, despite an increased incidence in this group of patients.
These findings are published in the March 9 issue of the journal Prostate Cancer and Prostatic Diseases (Nature). The study is led by Connor Hoge, a student at the UC College of Medicine, and Dr. Abhinav Sidana, director of urologic oncology and assistant professor in the Division of Urology at the UC College of Medicine. Sidana is also a UC Health urologist.
“Black men have a significantly higher incidence and are up to three times more likely to die of prostate cancer than white men,” says Sidana, corresponding author on this study. “MRI-ultrasound biopsy has emerged as a promising option for the detection of prostate cancer. In this study, we wanted to identify differences in use of MRI-ultrasound biopsy between black and white men with possible prostate cancer.”
Creating solutions for equitable health and well-being through research is one of the pathways outlined in UC’s strategic direction, Next Lives Here.
Dr. Abhinav Sidana, director of urologic oncology and assistant professor in the Division of Urology at the UC College of Medicine, during a prostate cancer procedure. Photo credit: Colleen Kelley/UC Creative Services
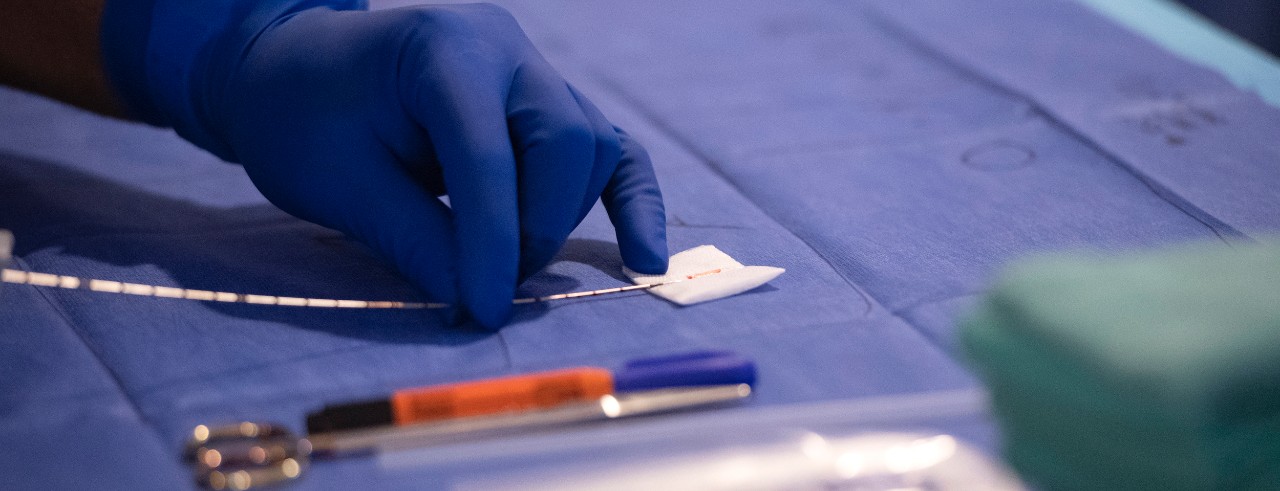
Sidana says the standard biopsy for men with suspicion of having prostate cancer is a random needle collection of between 12 to 40 samples from the prostate. However, because of the random nature of the collection, this can lead to overdiagnosis of prostate cancer where treatment is not needed, underdiagnosis prostate cancer where treatment is needed and a higher rate of tests that read negative for cancer when it is truly malignant.
With fusion biopsy, a navigation system similar to a GPS tracking device allows physicians to target biopsies to the exact suspicious location. MRI and ultrasound images are aligned and overlaid on real-time ultrasound to identify targets that are then labeled high, medium or low suspicion for cancer. This allows doctors to pinpoint the biopsy, meaning less sticks with a needle and more accurate samples.
Dr. Abhinav Sidana performs a prostate cancer biopsy. Photo credit: Colleen Kelley/UC Creative Services
The study included 619 men, of which 182 were African American and 437 were white; the patients were all treated at UC Medical Center. Forty-one (22.5%) African American men underwent MRI-ultrasound biopsy compared with 225 (51.5%) of white men.
“After adjusting for other factors, including age, race, prostate-specific antigen levels (which can determine risk for prostate cancer in the blood), other physical screening tactics, family history and health insurance providers, the odds of African American men having MRI-ultrasound biopsies were one-third the odds of white men having that type of biopsy,” says Sidana. “Although MRI-ultrasound biopsies are shown to be a better way to detect early-stage prostate cancer, we’re seeing this deficiency in a group of patients that would benefit the most from its use. We need to further investigate whether this difference is due to patient preference or if there are underlying socioeconomic, cultural or provider biases influencing this.”
Featured photo of prostate cancer biopsy by Colleen Kelley/UC Creative Services.
Next Lives Here
The University of Cincinnati is classified as a Research 1 institution by the Carnegie Commission and is ranked in the National Science Foundation's Top-35 public research universities. UC's graduate students and faculty investigate problems and innovate solutions with real-world impact. Next Lives Here.
Researchers cite no conflict of interest.
Related Stories
UC researcher launches app to connect patients to lifesaving...
May 7, 2025
A cardiologist and researcher at UC’s College of Medicine joined the Venture Lab at the 1819 Innovation Hub to launch High Enroll, an app that links clinical trials with willing participants.
The burning river that fueled a US green movement
May 5, 2025
An article by the BBC takes the reader back to the late 18th and 19th centuries, when US prosperity was defined by the industrial revolution, a time with little regard for the pollutants that came with industrial expansion. UC's David Stradling, professor of history, cited as expert source in the article.
Growing heart failure epidemic calls for prioritizing primary...
May 5, 2025
A rapidly growing heart failure epidemic calls for prioritizing primary prevention, according to a new scientific statement from the American Heart Association published in Circulation in April. The statement reviews the current evidence for predicting heart failure risk and offers risk-based strategies for heart failure prevention.
